Wed, May 27, 2026
Volume 14, Issue 4 (Autumn 2024)
PTJ 2024, 14(4): 311-320 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Rostami K D, Nabavinik M, Rezazadeh S. The Effect of Proprioceptive Neuromuscular Facilitation Exercise on Flexibility and Strength of Stroke Patients. PTJ 2024; 14 (4) :311-320
URL: http://ptj.uswr.ac.ir/article-1-614-en.html
URL: http://ptj.uswr.ac.ir/article-1-614-en.html
1- Department of Motor Behavior and Biomechanics, Faculty of Sports Sciences, University of Mazandaran, Babolsar, Iran.
2- Department of Sports Sciences, Faculty of Humanities, Shafagh Institute of Higher Education, Tonekabon, Iran.
2- Department of Sports Sciences, Faculty of Humanities, Shafagh Institute of Higher Education, Tonekabon, Iran.
Full-Text [PDF 570 kb]
(3340 Downloads)
| Abstract (HTML) (2898 Views)
Full-Text: (1557 Views)
Introduction
Stroke is one of the prevalent neurological issues in adults that compromises many aspects of life, such as quality of life (QoL) and functional capacity [1]. Despite improvements during inpatient rehabilitation, around 50–60% of stroke patients suffer long-term symptoms, such as weakness, atrophy, altered motor control due to denervation fatigability, remodeling disuse, and spasticity [2, 3].
Muscle weakness in the lower extremities and challenges in performing daily tasks are frequent issues following a stroke [4-6]. Furthermore, deficiencies in lower limb strength can hinder active engagement in various aspects of life for stroke survivors [7]. The inability of muscles to produce sufficient forces after a stroke can result in stretch reflex excitability [8, 9], increased coactivation of the antagonist muscle [10, 11, 12], reduced motor-unit firing rate [13, 14], and force deficits related to muscle length [15, 16]. Previous studies have demonstrated a strong and positive correlation between the strength of knee extensors on the paretic side and the strength of other muscle groups in stroke patients [4, 17].
Another complication following a stroke involves declined voluntary movement and decreased range of motion (ROM) of joints, frequently linked to increased resistance or stiffness, whether actively or passively. Stiffness can result from either “neural” or “non-neural” phenomena, including spastic dystonia, spasticity, soft-tissue fibrosis, and muscle contractures [18]. In stroke patients, the spasticity of plantar flexors can result in limited dorsiflexion ROM and the absence of posterior sliding of the talus. Inadequate dorsiflexion ROM of the ankle causes abnormal characteristics of gait, such as reduced speed of walking, unsymmetrical weight-bearing in the paralyzed leg, decreased rhythm, and greater possibility of falls [19, 20], thus, participating in activities of daily living would be limited in individuals with stroke [19]. Additionally, tightness in the hamstring causes posterior pelvic tilt, decreased lumbar lordosis, hamstring injuries, small step length, dynamic balance, and mobility disorders [21, 22]. According to the results of a systematic review, the benefits of proprioceptive neuromuscular facilitation (PNF) intervention on spasticity are limited [23].
Different therapeutic methods are suggested to reduce the symptoms of stroke patients, including stretch and strength training [24-26], biofeedback [26], virtual reality [27, 28], and mirror therapy [29].
PNF is one of the stretching techniques used to enhance the elasticity of muscle and has been reported to be effective for passive and active ROM, peak torque, and muscle strength [30]. PNF is frequently used in therapeutic exercises for stroke patients as an alternative to progressive resistance exercise to avoid injury [31].
Previous studies have demonstrated that PNF exercises can improve sensory motor function [32], functional outcome and QoL [33], balance and walking ability [31], muscle tone, and stiffness [34] in stroke patients; however, rare information exists regarding the efficacy of PNF exercises on muscle flexibility and strength of stroke patients. Therefore, the current study was conducted to examine the effect of PNF exercise on the flexibility of the gastrocnemius and the hamstring, and the strength of the hamstring and quadriceps muscles. We hypothesized that PNF exercises can increase flexibility and strength of lower extremity muscles in stroke.
Materials and Methods
Twenty-four male patients with stroke aged between 40 to 70 years participated in this study (Table 1).
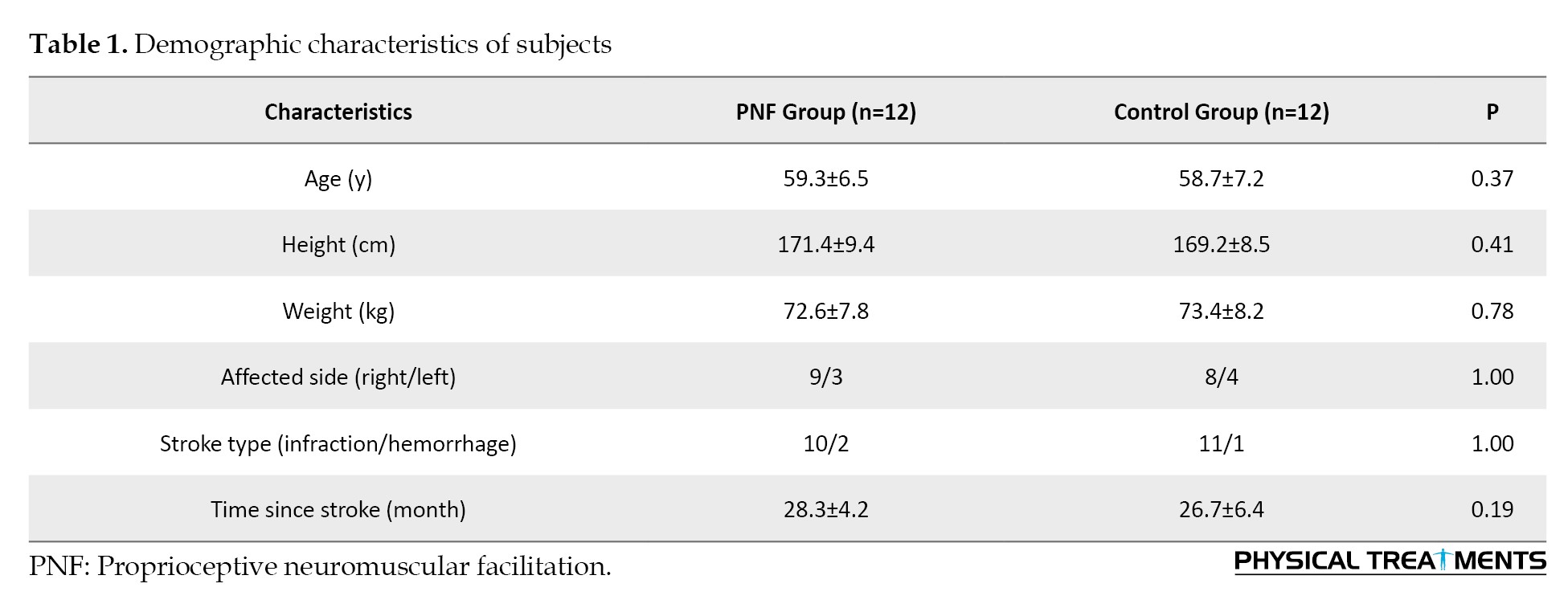
A sample size estimate was performed by G*Power software, version 3.1 and indicated that 24 subjects are necessary to reach an a priori power of 0.80. The participants were included in the study based on confirmation of stroke through magnetic resonance imaging (MRI) or computed tomography (CT) scans, occurrence of unilateral stroke, presence of gastrocnemius muscle tightness, ability to independently walk 10 meters, and achieving a score of 24 or more on the mini-mental state examination to ensure comprehension and ability to follow the researcher’s instructions. Patients with cognitive disorders, inability to execute tests or other chronic health conditions were excluded from the study. They were then randomized using a random number generator into two groups, a control group (n=12) and a PNF group (n=12), which received PNF exercises (Figure 1).
Subjects signed written informed consent to attend to the study.
Intervention
All patients performed their conventional rehabilitation, including mobilization, balance, strengthening, ambulating, and gait training for 30 minutes, and three times weekly. The PNF group additionally received the contract-relax (CR) technique [30] of PNF stretching for gastrocnemius and hamstring muscles for 20 minutes and three times weekly. For PNF stretching of the gastrocnemius muscle, the participant was placed in a lying back position, and the therapist moved the ankle in the direction of dorsiflexion to the point of discomfort. Then the patient performed maximal isometric contraction of the gastrocnemius muscle against therapist resistance and maintained this position for 5 s. After holding the isometric contraction, the therapist asked the patient to relax for 10 s and the foot was repositioned in the new range. Then the foot was moved to the new barrier point and the procedure was repeated.
During hamstring PNF stretching, the participant was positioned lying back, and the therapist raised the hip joint to the point of discomfort while maintaining full extension of the opposite hip and knee joints, as well as the ipsilateral knee joint. Then, the patient engages in a maximum isometric contraction of the hamstring for 5 s, followed by a 10-s rest period. Afterward, the therapist increases the hip flexion range. PNF stretching is exclusively performed on the paretic side, with four sets of PNF stretching for each muscle, separated by 30 s rest intervals [35].
Gastrocnemius and hamstring flexibility measurement
Weight-bearing lunge test has been applied to evaluate dorsiflexion ROM using a tape measure stoke on the ground and wall. A vertical line has been drowned on the wall perpendicular to the tape measure. Patients were instructed to face the wall and then perform forward lunges until their forward knee touched the wall while keeping the calcaneus of the tested leg on the floor. Then the examiner measured (cm) the distance between the wall and the tip of the big toe. The distance can be increased since the patients can touch the wall with the knee while keeping the heel placed on the floor [36]. The test was performed three times for each patient and the best-recorded trial was used for analysis.
The weight-bearing lunge test demonstrated acceptable inter-rater reliability (R=0.99, 95% CI, 0.97%, 0.99%) [36] and excellent intra-rater reliability, with intraclass correlation coefficient (ICC) values ranging from 0.98 to 0.99 [36, 37].
For the assessment of hamstring flexibility, the active straight leg raise (aSLR) test was utilized. During this test, the patient is placed in a lying back position and instructed to bend the hip joint until further flexion becomes unbearable. Throughout the maneuver, the same knee joint and opposite hip and knee joints are kept in the extended position to avoid the posterior tilt of the pelvic. The examiner measured the angle with a goniometer [38]. The intraclass correlation coefficient (ICC) reported for the aSLR test ranges from 0.93 to 0.97, indicating excellent intra-rater reliability [39].
Knee flexors and extensors strength measurement
The hand-held dynamometer (Commander Echo™ Muscle Testing Dynamometer, JTECH Medical Corp, USA) was used to assess the strength of knee flexors and extensors. The participant seated on the edge of the table while the feet and back were free to move, the hip and knee joints were kept to 90◦ flexion, to stabilize the body and the hands grasping the sides of the table, and the examiner held the dynamometer on the anterior/posterior of the leg above the ankle. First, three familiarization trials (submaximally) were performed and then, three maximal testing trials were implemented. Each measurement lasted for 5 s and was followed by a 30 s rest time. The force was increased slowly by the participant during a three to five-second max effort push into the dynamometer against the examiner’s resistance. The examiner provided verbal encouragement to ensure that maximal effort was achieved [40].
Statistical analysis
The normal distribution of data was verified by the Shapiro-Wilk test. To analyze the impact of PNF stretch on flexibility and strength, a 2×2 mixed-model repeated measures analysis of variance (ANOVA) was conducted, with time as the within-subject factor and group (experimental and control) as the between-subject factor. Additionally, univariate tests, including independent and paired t-tests, were conducted to determine group differences in the presence of significant interactions and main effects. Statistical analyses were conducted with SPSS software, version 27 (IBM Corporation) and the significance level was set at P<0.05.
Results
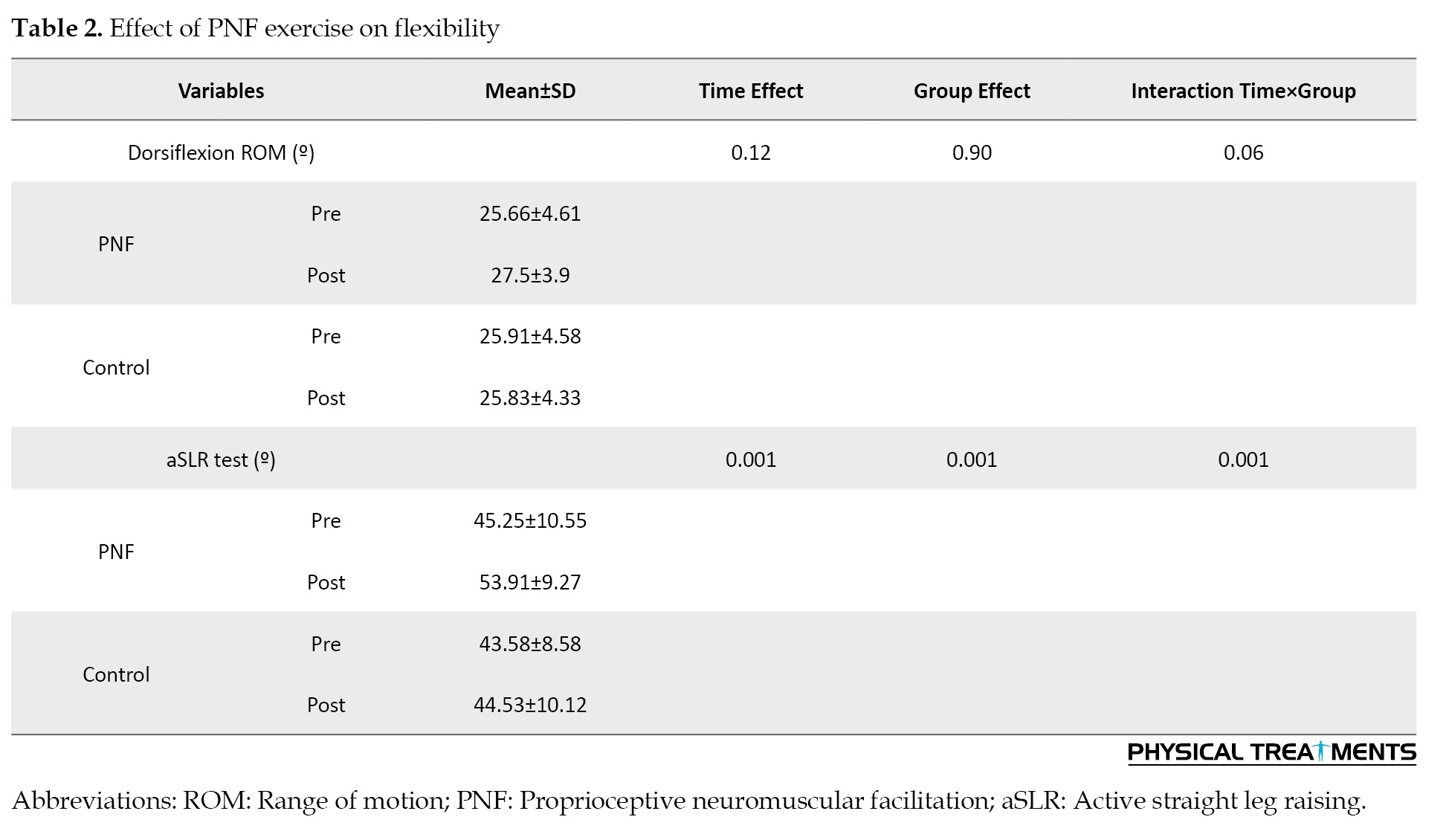
Table 1 presents the patients’ characteristics, including age, height, weight, stroke type, affected side, and time since stroke. No significant difference was observed in patient characteristics.
Flexibility
The significant effect of time (F=63.57, P<0.01) group (F=37.46, P<0.01) and interaction of time×group (F=33.24, P<0.01) was observed for hamstring flexibility. Follow-up tests showed that significant increase of the aSLR (effect size=0.75) in the PNF group. No significant interactions or main effects were found for gastrocnemius flexibility in the wall lung test (Table 2).
Strength
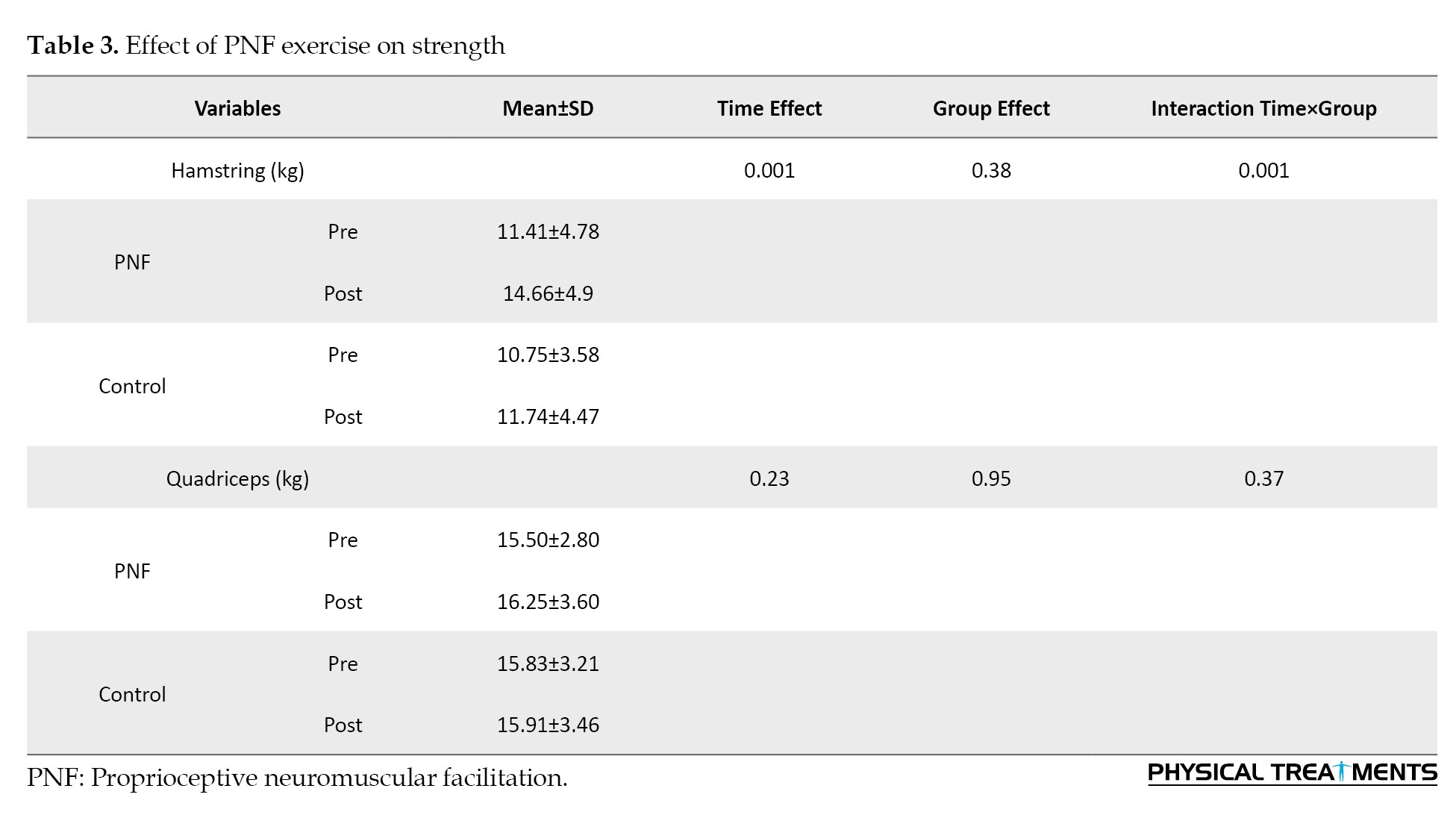
A significant effect of time (F=54.85, P<0.01) and interaction of time×group (F=23.86, P<0.01) was observed for hamstring strength. Follow-up tests revealed a significant increase in hamstring muscle strength (effect size=0.67) in the PNF group after exercise. Interactions or main effects were not significant for quadriceps strength (Table 3).
Discussion
The current study was conducted to examine the effectiveness of PNF exercise on flexibility and strength in stroke patients. We hypothesized that PNF exercise increases the flexibility and strength of the patients after stroke. Our results only support the effect of PNF exercise on hamstring muscle flexibility and strength.
The aSLR increased after PNF exercise in stroke patients, indicating increased flexibility of hamstring muscle after PNF exercise. Hamstring flexibility is a crucial physiological factor and poor hamstring flexibility can result in injuries, musculoskeletal dysfunction, and decreased physical function [41]. Previous studies have demonstrated that neurodynamic sliding technique [42] and dynamic soft tissue mobilization [41] increase hamstring flexibility in stroke patients; however, little knowledge exists regarding the effect of the PNF exercise on hamstring muscle flexibility after stroke. Four theories exist about the effect of PNF contract-relax (CR) method to improve ROM, including reciprocal inhibition, autogenic inhibition, gate control, and the stress relaxation theory [43, 44]. These mechanisms involve reflexes triggered by Golgi tendon organs (GTOs) located in the tendons of the target muscle (TM) or the antagonist muscle to the TM, detecting detrimental stimuli. In this study, we utilized inhibition of the TM (hamstring) to enhance the ROM. In the CR method, the isometric contraction of the TM leads to autogenic inhibition within the TM, reducing its excitability due to inhibitory signals from GTOs. GTOs serve a protective function, inducing relaxation of the TM, which leverages the viscoelastic properties of the musculotendinous units. This allows for “creeping” of the muscle and facilitates further stretching of the TM, thereby contributing to the observed increases in ROM and flexibility resulting from PNF stretching [43]. The effect size for increasing hamstring muscle flexibility was 0.75, which indicates a strong effect based on Cohen’s d [45].
The results of this study indicated a significant increase in knee flexor strength after PNF exercises. Muscle weaknesses of the lower limbs are the most common sign after stroke [46]. The mechanism of changes in the structure and function of the hamstring group after stroke can be due to the retention of neuromuscular connection coupled with reduced neuromuscular activation and muscular unloading. Hence, hamstring group weakness results from neural, structural, and mechanical changes in this group of muscles [47]. Previous studies investigated the effects of resistance training [48, 49], electrical stimulation cycling [50], and sit-to-stand training [51, 52] on plantar flexors and knee extensor strength in individuals with stroke. However, it has been indicated that PNF exercise can be a good replacement for resistance training in improving muscle strength [30, 53]. The results of the present study can add extra support for the possible role of PNF exercise in improving knee flexor strength after stroke. The PNF technique relies on using a fusional stimulus to activate neural muscle receptors, which in turn increase the activation of motor units in series, leading to enhanced muscle strength [54].
No significant change was observed in gastrocnemius flexibility and knee extensor strength after PNF exercise. It has been demonstrated that the effect of stretching exercises varies according to the joint. Thus, it is not possible to explain the functional effects between different joints [55]. In addition, each muscle group responds differently to stretching based on the level of stiffness. Studies reported a greater level of gastrocnemius (especially medial gastrocnemius) stiffness in stroke patients [56, 57], this could explain why our PNF exercise did not change the gastrocnemius muscle flexibility.
This study had some limitations. We had a small sample size in each group which could affect our results. We only used hamstring muscle isometric contraction (CR) to improve the ROM. Other PNF methods may have different results. Additionally, other functional tests may better reflect lower extremity flexibility and strength. Moreover, studies with long-time follow-up are required to evaluate the sustainability of the PNF exercises. Finally, the current study recruited only male stroke patients and the results cannot be generalized to women.
Conclusion
The study’s main discovery is that an 8-week PNF stretch program can boost hamstring flexibility and strength in stroke patients, even after 2 years. This suggests that including PNF stretching exercises in the rehabilitation of stroke survivors can benefit their hamstring muscle properties.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Institutional Ethics Committee of Shahrood University of Technology (Code: IR.SHAHROODUT.REC-1402.22). The subjects provided informed consent to participate in this research.
Funding
This research received no specific grant from funding agencies in public, commercial, or not-for-profit sectors.
Authors' contributions
Supervision and data analysis: Komeil Dashti Rostami and Mahdi Nabavi Nik; Writing-original draft, review and editing: Komeil Dashti Rostami; Data collection: Shahram Rezazadeh; Conceptualization and Methodology: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
Authors would like to thank all participants for their cooperation in conducting this study.
References
Stroke is one of the prevalent neurological issues in adults that compromises many aspects of life, such as quality of life (QoL) and functional capacity [1]. Despite improvements during inpatient rehabilitation, around 50–60% of stroke patients suffer long-term symptoms, such as weakness, atrophy, altered motor control due to denervation fatigability, remodeling disuse, and spasticity [2, 3].
Muscle weakness in the lower extremities and challenges in performing daily tasks are frequent issues following a stroke [4-6]. Furthermore, deficiencies in lower limb strength can hinder active engagement in various aspects of life for stroke survivors [7]. The inability of muscles to produce sufficient forces after a stroke can result in stretch reflex excitability [8, 9], increased coactivation of the antagonist muscle [10, 11, 12], reduced motor-unit firing rate [13, 14], and force deficits related to muscle length [15, 16]. Previous studies have demonstrated a strong and positive correlation between the strength of knee extensors on the paretic side and the strength of other muscle groups in stroke patients [4, 17].
Another complication following a stroke involves declined voluntary movement and decreased range of motion (ROM) of joints, frequently linked to increased resistance or stiffness, whether actively or passively. Stiffness can result from either “neural” or “non-neural” phenomena, including spastic dystonia, spasticity, soft-tissue fibrosis, and muscle contractures [18]. In stroke patients, the spasticity of plantar flexors can result in limited dorsiflexion ROM and the absence of posterior sliding of the talus. Inadequate dorsiflexion ROM of the ankle causes abnormal characteristics of gait, such as reduced speed of walking, unsymmetrical weight-bearing in the paralyzed leg, decreased rhythm, and greater possibility of falls [19, 20], thus, participating in activities of daily living would be limited in individuals with stroke [19]. Additionally, tightness in the hamstring causes posterior pelvic tilt, decreased lumbar lordosis, hamstring injuries, small step length, dynamic balance, and mobility disorders [21, 22]. According to the results of a systematic review, the benefits of proprioceptive neuromuscular facilitation (PNF) intervention on spasticity are limited [23].
Different therapeutic methods are suggested to reduce the symptoms of stroke patients, including stretch and strength training [24-26], biofeedback [26], virtual reality [27, 28], and mirror therapy [29].
PNF is one of the stretching techniques used to enhance the elasticity of muscle and has been reported to be effective for passive and active ROM, peak torque, and muscle strength [30]. PNF is frequently used in therapeutic exercises for stroke patients as an alternative to progressive resistance exercise to avoid injury [31].
Previous studies have demonstrated that PNF exercises can improve sensory motor function [32], functional outcome and QoL [33], balance and walking ability [31], muscle tone, and stiffness [34] in stroke patients; however, rare information exists regarding the efficacy of PNF exercises on muscle flexibility and strength of stroke patients. Therefore, the current study was conducted to examine the effect of PNF exercise on the flexibility of the gastrocnemius and the hamstring, and the strength of the hamstring and quadriceps muscles. We hypothesized that PNF exercises can increase flexibility and strength of lower extremity muscles in stroke.
Materials and Methods
Twenty-four male patients with stroke aged between 40 to 70 years participated in this study (Table 1).

A sample size estimate was performed by G*Power software, version 3.1 and indicated that 24 subjects are necessary to reach an a priori power of 0.80. The participants were included in the study based on confirmation of stroke through magnetic resonance imaging (MRI) or computed tomography (CT) scans, occurrence of unilateral stroke, presence of gastrocnemius muscle tightness, ability to independently walk 10 meters, and achieving a score of 24 or more on the mini-mental state examination to ensure comprehension and ability to follow the researcher’s instructions. Patients with cognitive disorders, inability to execute tests or other chronic health conditions were excluded from the study. They were then randomized using a random number generator into two groups, a control group (n=12) and a PNF group (n=12), which received PNF exercises (Figure 1).
Subjects signed written informed consent to attend to the study.
Intervention
All patients performed their conventional rehabilitation, including mobilization, balance, strengthening, ambulating, and gait training for 30 minutes, and three times weekly. The PNF group additionally received the contract-relax (CR) technique [30] of PNF stretching for gastrocnemius and hamstring muscles for 20 minutes and three times weekly. For PNF stretching of the gastrocnemius muscle, the participant was placed in a lying back position, and the therapist moved the ankle in the direction of dorsiflexion to the point of discomfort. Then the patient performed maximal isometric contraction of the gastrocnemius muscle against therapist resistance and maintained this position for 5 s. After holding the isometric contraction, the therapist asked the patient to relax for 10 s and the foot was repositioned in the new range. Then the foot was moved to the new barrier point and the procedure was repeated.
During hamstring PNF stretching, the participant was positioned lying back, and the therapist raised the hip joint to the point of discomfort while maintaining full extension of the opposite hip and knee joints, as well as the ipsilateral knee joint. Then, the patient engages in a maximum isometric contraction of the hamstring for 5 s, followed by a 10-s rest period. Afterward, the therapist increases the hip flexion range. PNF stretching is exclusively performed on the paretic side, with four sets of PNF stretching for each muscle, separated by 30 s rest intervals [35].
Gastrocnemius and hamstring flexibility measurement
Weight-bearing lunge test has been applied to evaluate dorsiflexion ROM using a tape measure stoke on the ground and wall. A vertical line has been drowned on the wall perpendicular to the tape measure. Patients were instructed to face the wall and then perform forward lunges until their forward knee touched the wall while keeping the calcaneus of the tested leg on the floor. Then the examiner measured (cm) the distance between the wall and the tip of the big toe. The distance can be increased since the patients can touch the wall with the knee while keeping the heel placed on the floor [36]. The test was performed three times for each patient and the best-recorded trial was used for analysis.
The weight-bearing lunge test demonstrated acceptable inter-rater reliability (R=0.99, 95% CI, 0.97%, 0.99%) [36] and excellent intra-rater reliability, with intraclass correlation coefficient (ICC) values ranging from 0.98 to 0.99 [36, 37].
For the assessment of hamstring flexibility, the active straight leg raise (aSLR) test was utilized. During this test, the patient is placed in a lying back position and instructed to bend the hip joint until further flexion becomes unbearable. Throughout the maneuver, the same knee joint and opposite hip and knee joints are kept in the extended position to avoid the posterior tilt of the pelvic. The examiner measured the angle with a goniometer [38]. The intraclass correlation coefficient (ICC) reported for the aSLR test ranges from 0.93 to 0.97, indicating excellent intra-rater reliability [39].
Knee flexors and extensors strength measurement
The hand-held dynamometer (Commander Echo™ Muscle Testing Dynamometer, JTECH Medical Corp, USA) was used to assess the strength of knee flexors and extensors. The participant seated on the edge of the table while the feet and back were free to move, the hip and knee joints were kept to 90◦ flexion, to stabilize the body and the hands grasping the sides of the table, and the examiner held the dynamometer on the anterior/posterior of the leg above the ankle. First, three familiarization trials (submaximally) were performed and then, three maximal testing trials were implemented. Each measurement lasted for 5 s and was followed by a 30 s rest time. The force was increased slowly by the participant during a three to five-second max effort push into the dynamometer against the examiner’s resistance. The examiner provided verbal encouragement to ensure that maximal effort was achieved [40].
Statistical analysis
The normal distribution of data was verified by the Shapiro-Wilk test. To analyze the impact of PNF stretch on flexibility and strength, a 2×2 mixed-model repeated measures analysis of variance (ANOVA) was conducted, with time as the within-subject factor and group (experimental and control) as the between-subject factor. Additionally, univariate tests, including independent and paired t-tests, were conducted to determine group differences in the presence of significant interactions and main effects. Statistical analyses were conducted with SPSS software, version 27 (IBM Corporation) and the significance level was set at P<0.05.
Results
Table 1 presents the patients’ characteristics, including age, height, weight, stroke type, affected side, and time since stroke. No significant difference was observed in patient characteristics.
Flexibility
The significant effect of time (F=63.57, P<0.01) group (F=37.46, P<0.01) and interaction of time×group (F=33.24, P<0.01) was observed for hamstring flexibility. Follow-up tests showed that significant increase of the aSLR (effect size=0.75) in the PNF group. No significant interactions or main effects were found for gastrocnemius flexibility in the wall lung test (Table 2).

Strength
A significant effect of time (F=54.85, P<0.01) and interaction of time×group (F=23.86, P<0.01) was observed for hamstring strength. Follow-up tests revealed a significant increase in hamstring muscle strength (effect size=0.67) in the PNF group after exercise. Interactions or main effects were not significant for quadriceps strength (Table 3).

Discussion
The current study was conducted to examine the effectiveness of PNF exercise on flexibility and strength in stroke patients. We hypothesized that PNF exercise increases the flexibility and strength of the patients after stroke. Our results only support the effect of PNF exercise on hamstring muscle flexibility and strength.
The aSLR increased after PNF exercise in stroke patients, indicating increased flexibility of hamstring muscle after PNF exercise. Hamstring flexibility is a crucial physiological factor and poor hamstring flexibility can result in injuries, musculoskeletal dysfunction, and decreased physical function [41]. Previous studies have demonstrated that neurodynamic sliding technique [42] and dynamic soft tissue mobilization [41] increase hamstring flexibility in stroke patients; however, little knowledge exists regarding the effect of the PNF exercise on hamstring muscle flexibility after stroke. Four theories exist about the effect of PNF contract-relax (CR) method to improve ROM, including reciprocal inhibition, autogenic inhibition, gate control, and the stress relaxation theory [43, 44]. These mechanisms involve reflexes triggered by Golgi tendon organs (GTOs) located in the tendons of the target muscle (TM) or the antagonist muscle to the TM, detecting detrimental stimuli. In this study, we utilized inhibition of the TM (hamstring) to enhance the ROM. In the CR method, the isometric contraction of the TM leads to autogenic inhibition within the TM, reducing its excitability due to inhibitory signals from GTOs. GTOs serve a protective function, inducing relaxation of the TM, which leverages the viscoelastic properties of the musculotendinous units. This allows for “creeping” of the muscle and facilitates further stretching of the TM, thereby contributing to the observed increases in ROM and flexibility resulting from PNF stretching [43]. The effect size for increasing hamstring muscle flexibility was 0.75, which indicates a strong effect based on Cohen’s d [45].
The results of this study indicated a significant increase in knee flexor strength after PNF exercises. Muscle weaknesses of the lower limbs are the most common sign after stroke [46]. The mechanism of changes in the structure and function of the hamstring group after stroke can be due to the retention of neuromuscular connection coupled with reduced neuromuscular activation and muscular unloading. Hence, hamstring group weakness results from neural, structural, and mechanical changes in this group of muscles [47]. Previous studies investigated the effects of resistance training [48, 49], electrical stimulation cycling [50], and sit-to-stand training [51, 52] on plantar flexors and knee extensor strength in individuals with stroke. However, it has been indicated that PNF exercise can be a good replacement for resistance training in improving muscle strength [30, 53]. The results of the present study can add extra support for the possible role of PNF exercise in improving knee flexor strength after stroke. The PNF technique relies on using a fusional stimulus to activate neural muscle receptors, which in turn increase the activation of motor units in series, leading to enhanced muscle strength [54].
No significant change was observed in gastrocnemius flexibility and knee extensor strength after PNF exercise. It has been demonstrated that the effect of stretching exercises varies according to the joint. Thus, it is not possible to explain the functional effects between different joints [55]. In addition, each muscle group responds differently to stretching based on the level of stiffness. Studies reported a greater level of gastrocnemius (especially medial gastrocnemius) stiffness in stroke patients [56, 57], this could explain why our PNF exercise did not change the gastrocnemius muscle flexibility.
This study had some limitations. We had a small sample size in each group which could affect our results. We only used hamstring muscle isometric contraction (CR) to improve the ROM. Other PNF methods may have different results. Additionally, other functional tests may better reflect lower extremity flexibility and strength. Moreover, studies with long-time follow-up are required to evaluate the sustainability of the PNF exercises. Finally, the current study recruited only male stroke patients and the results cannot be generalized to women.
Conclusion
The study’s main discovery is that an 8-week PNF stretch program can boost hamstring flexibility and strength in stroke patients, even after 2 years. This suggests that including PNF stretching exercises in the rehabilitation of stroke survivors can benefit their hamstring muscle properties.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Institutional Ethics Committee of Shahrood University of Technology (Code: IR.SHAHROODUT.REC-1402.22). The subjects provided informed consent to participate in this research.
Funding
This research received no specific grant from funding agencies in public, commercial, or not-for-profit sectors.
Authors' contributions
Supervision and data analysis: Komeil Dashti Rostami and Mahdi Nabavi Nik; Writing-original draft, review and editing: Komeil Dashti Rostami; Data collection: Shahram Rezazadeh; Conceptualization and Methodology: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
Authors would like to thank all participants for their cooperation in conducting this study.
References
- Carr JH, Shepherd RB. Neurological rehabilitation: Optimizing motor performance. Amsterdam: Elsevier Health Sciences; 2010. [Link]
- Schaechter JD. Motor rehabilitation and brain plasticity after hemiparetic stroke. Progress in Neurobiology. 2004; 73(1):61-72. [DOI:10.1016/j.pneurobio.2004.04.001] [PMID]
- Scherbakov N, Von Haehling S, Anker SD, Dirnagl U, Doehner W. Stroke induced Sarcopenia: muscle wasting and disability after stroke. International Journal of Cardiology. 2013; 170(2):89-94. [DOI:10.1016/j.ijcard.2013.10.031] [PMID]
- Aguiar LT, Camargo LBA, Estarlino LD, Teixeira-Salmela LF, Faria CDCM. Strength of the lower limb and trunk muscles is associated with gait speed in individuals with sub-acute stroke: a cross-sectional study. Brazilian Journal of Physical Therapy. 2018; 22(6):459-66. [DOI:10.1016/j.bjpt.2018.03.001] [PMID]
- Hyun CW, Han EY, Im SH, Choi JC, Kim BR, Yoon HM, et al. Hemiparetic knee extensor strength and balance function are predictors of ambulatory function in subacute stroke patients. Annals of Rehabilitation Medicine. 2015; 39(4):577-85. [DOI:10.5535/arm.2015.39.4.577] [PMID]
- Ng SS, Shepherd RB. Weakness in patients with stroke: Implications for strength training in neurorehabilitation. Physical Therapy Reviews. 2000; 5(4):227-38. [DOI:10.1179/108331900786166650]
- Faria-Fortini I, Basílio ML, Polese JC, Menezes KKP, Faria CDCM, Scianni AA, et al. Strength deficits of the paretic lower extremity muscles were the impairment variables that best explained restrictions in participation after stroke. Disability and Rehabilitation. 2017; 39(21):2158-63. [DOI:10.1080/09638288.2016.1219397] [PMID]
- Corcos DM, Gottlieb GL, Penn RD, Myklebust B, Agarwal GC. Movement deficits caused by hyperexcitable stretch reflexes in spastic humans. Brain. 1986; 109(5):1043-58. [DOI:10.1093/brain/109.5.1043] [PMID]
- Levin MF, Selles RW, Verheul MH, Meijer OG. Deficits in the coordination of agonist and antagonist muscles in stroke patients: implications for normal motor control. Brain Research. 2000; 853(2):352-69. [DOI:10.1016/S0006-8993(99)02298-2] [PMID]
- Fellows SJ, Kaus C, Ross HF, Thilmann AF. Agonist and antagonist EMG activation during isometric torque development at the elbow in spastic hemiparesis. Electroencephalography and Clinical Neurophysiology/Evoked Potentials Section. 1994; 93(2):106-12. [DOI:10.1016/0168-5597(94)90073-6] [PMID]
- El-Abd M, Ibrahim I, Dietz V. Impaired activation pattern in antagonistic elbow muscles of patients with spastic hemiparesis: Contribution to movement disorder. Electromyography and Clinical Neurophysiology. 1993; 33(4):247-55. [PMID]
- Jakobsson F, Grimby L, Edström L. Motoneuron activity and muscle fibre type composition in hemiparesis. Journal of Rehabilitation Medicine. 1992; 24(3):115-9. [DOI:10.2340/1650197792115119]
- Gemperline JJ, Allen S, Walk D, Rymer WZ. Characteristics of motor unit discharge in subjects with hemiparesis. Muscle & Nerve. 1995; 18(10):1101-14. [DOI:10.1002/mus.880181006] [PMID]
- Frontera WR, Grimby L, Larsson L. Firing rate of the lower motoneuron and contractile properties of its muscle fibers after upper motoneuron lesion in man. Muscle & Nerve: Official Journal of the American Association of Electrodiagnostic Medicine. 1997; 20(8):938-47. [PMID]
- Ada L, Canning C, Dwyer T. Effect of muscle length on strength and dexterity after stroke. Clinical Rehabilitation. 2000; 14(1):55-61. [DOI:10.1191/026921500671430626] [PMID]
- Koo TK, Mak AF, Hung L, Dewald JP. Joint position dependence of weakness during maximum isometric voluntary contractions in subjects with hemiparesis. Archives of Physical Medicine and Rehabilitation. 2003; 84(9):1380-6. [DOI:10.1016/S0003-9993(03)00238-7] [PMID]
- Bohannon RW, Andrews AW. Relationships between impairments in strength of limb muscle actions following stroke. Perceptual and Motor Skills. 1998; 87(3_suppl):1327-30. [DOI:10.2466/pms.1998.87.3f.1327] [PMID]
- Lecharte T, Gross R, Nordez A, Le Sant G. Effect of chronic stretching interventions on the mechanical properties of muscles in patients with stroke: A systematic review. Annals of Physical and Rehabilitation Medicine. 2020; 63(3):222-9. [DOI:10.1016/j.rehab.2019.12.003] [PMID]
- Ravichandran H, Janakiraman B. The effects of ankle joint mobilization on dorsiflexion range and gait parameters in chronic stroke survivors: A systematic review and meta-analysis. Journal of Stroke Medicine. 2021; 4(1):15-24. [DOI:10.1177/2516608520982874]
- Young R, Nix S, Wholohan A, Bradhurst R, Reed L. Interventions for increasing ankle joint dorsiflexion: A systematic review and meta-analysis. Journal of Foot and Ankle Research. 2013; 6(1):1-10. [DOI:10.1186/1757-1146-6-46]
- Ahmed AR, Samhan AF. Short term effects of neurodynamic stretching and static stretching techniques on hamstring muscle flexibility in healthy male subjects. International Journal of Medical Research & Health Sciences. 2016; 5(5):36-41. [Link]
- Encarnación-Martínez A, García-Gallart A, Pérez-Soriano P, Catalá-Vilaplana I, Rizo-Albero J, Sanchis-Sanchis R. Effect of hamstring tightness and fatigue on dynamic stability and agility in physically active young men. Sensors. 2023; 23(3):1633. [DOI:10.3390/s23031633] [PMID]
- Alashram AR, Alghwiri AA, Padua E, Annino G. Efficacy of proprioceptive neuromuscular facilitation on spasticity in patients with stroke: A systematic review. Physical Therapy Reviews. 2021; 26(3):168-76. [DOI:10.1080/10833196.2021.1892281]
- Patten C, Condliffe EG, Dairaghi CA, Lum PS. Concurrent neuromechanical and functional gains following upper-extremity power training post-stroke. Journal of Neuroengineering and Rehabilitation. 2013; 10:1. [DOI:10.1186/1743-0003-10-1] [PMID]
- Ghasemi E, Khademi-Kalantari K, Khalkhali-Zavieh M, Rezasoltani A, Ghasemi M, Akbarzadeh Baghban A, et al. The effect of functional stretching exercises on neural and mechanical properties of the spastic medial gastrocnemius muscle in patients with chronic stroke: A randomized controlled trial. Journal of Stroke and Cerebrovascular Diseases. 2018; 27(7):1733-42. [DOI:10.1016/j.jstrokecerebrovasdis.2018.01.024] [PMID]
- Bressel E, McNair PJ. The effect of prolonged static and cyclic stretching on ankle joint stiffness, torque relaxation, and gait in people with stroke. Physical Therapy. 2002; 82(9):880-7. [DOI:10.1093/ptj/82.9.880] [PMID]
- Turolla A, Dam M, Ventura L, Tonin P, Agostini M, Zucconi C, et al. Virtual reality for the rehabilitation of the upper limb motor function after stroke: A prospective controlled trial. Journal of Neuroengineering and Rehabilitation. 2013; 10:85. [DOI:10.1186/1743-0003-10-85] [PMID]
- Smith C, Read J, Bennie C, Hale L, Milosavljevic S. Can non-immersive virtual reality improve physical outcomes of rehabilitation? Physical Therapy Reviews. 2012; 17(1):1-15. [DOI:10.1179/1743288X11Y.0000000047]
- Lee MM, Cho HY, Song CH. The mirror therapy program enhances upper-limb motor recovery and motor function in acute stroke patients. American Journal of Physical Medicine & Rehabilitation. 2012; 91(8):689-96, quiz 697-700. [DOI:10.1097/PHM.0b013e31824fa86d] [PMID]
- Hindle KB, Whitcomb TJ, Briggs WO, Hong J. Proprioceptive neuromuscular facilitation (PNF): Its mechanisms and effects on range of motion and muscular function. Journal of Human Kinetics. 2012; 31:105-13. [DOI:10.2478/v10078-012-0011-y] [PMID]
- Kim Y, Kim E, Gong W. The effects of trunk stability exercise using PNF on the functional reach test and muscle activities of stroke patients. Journal of Physical Therapy Science. 2011; 23(5):699-702. [DOI:10.1589/jpts.23.699]
- Junior VADS, Santos MS, Ribeiro NMDS, Maldonado IL. Combining proprioceptive neuromuscular facilitation and virtual reality for improving sensorimotor function in stroke survivors: a randomized clinical trial. Journal of Central Nervous System Disease. 2019; 11:1179573519863826.[DOI:10.1177/1179573519863826] [PMID]
- Chaturvedi P, Tiwari V, Singh AK, Kulshrestha D, Kumar Maurya P, Thacker AK. Effects of early proprioceptive neuromuscular facilitation exercises on functional outcome and quality of life in patients with stroke. MGM Journal of Medical Sciences. 2017; 4(3):130-3. [Link]
- Wang JS, Lee SB, Moon SH. The immediate effect of PNF pattern on muscle tone and muscle stiffness in chronic stroke patient. Journal of Physical Therapy Science. 2016; 28(3):967-70. [DOI:10.1589/jpts.28.967] [PMID]
- Bradley PS, Olsen PD, Portas MD. The effect of static, ballistic, and proprioceptive neuromuscular facilitation stretching on vertical jump performance. The Journal of Strength & Conditioning Research. 2007; 21(1):223-6. [DOI:10.1519/00124278-200702000-00040] [PMID]
- Bennell K, Talbot R, Wajswelner H, Techovanich W, Kelly D, Hall AJ. Intra-rater and inter-rater reliability of a weight-bearing lunge measure of ankle dorsiflexion. Australian Journal of Physiotherapy. 1998; 44(3):175-80. [DOI:10.1016/S0004-9514(14)60377-9] [PMID]
- Dennis RJ, Finch CF, Elliott BC, Farhart PJ. The reliability of musculoskeletal screening tests used in cricket. Physical Therapy in Sport. 2008; 9(1):25-33. [DOI:10.1016/j.ptsp.2007.09.004] [PMID]
- Medeiros DM, Miranda LLP, Marques VB, de Araujo Ribeiro-Alvares JB, Baroni BM. Accuracy of the functional movement screen (fmstm) active straight leg raise test to evaluate hamstring flexibility in soccer players. International Journal of Sports Physical Therapy. 2019; 14(6):877-84. [DOI:10.26603/ijspt20190877] [PMID]
- Neto T, Jacobsohn L, Carita AI, Oliveira R. Reliability of the active-knee-extension and straight-leg-raise tests in subjects with flexibility deficits. Journal of Sport Rehabilitation. 2015; 24(4):2014-0220. [DOI:10.1123/jsr.2014-0220] [PMID]
- Aguiar LT, Martins JC, de Brito SAF, Mendes CLG, Teixeira-Salmela LF, Faria CDCDM. Knee extensor muscles strength indicates global lower-limb strength in individuals who have suffered a stroke: A cross-sectional study. Brazilian Journal of Physical Therapy. 2019; 23(3):221-7. [DOI:10.1016/j.bjpt.2018.08.001] [PMID]
- Suhail M, Prakash A, Sonali D, Sangeeta M. Effectiveness of dynamic soft tissue mobilization vs passive stretching to improve hamstring flexibility in stroke patients-A comparative study. International Journal of Physical Education, Sports and Health. 2022; 9(1):345-9. [Link]
- Anandhraj J, Kumaresan A. Effect of neurodynamic sliding technique on hemiplegic stroke subjects with hamstring tightness. Indian Journal of Public Health Research & Development. 2020; 11(1):251-4. [DOI:10.37506/v11/i1/2020/ijphrd/193824]
- Sharman MJ, Cresswell AG, Riek S. Proprioceptive neuromuscular facilitation stretching: Mechanisms and clinical implications. Sports Medicine. 2006; 36(11):929-39.[DOI:10.2165/00007256-200636110-00002] [PMID]
- Rowlands AV, Marginson VF, Lee J. Chronic flexibility gains: Effect of isometric contraction duration during proprioceptive neuromuscular facilitation stretching techniques. Research Quarterly for Exercise and Sport. 2003; 74(1):47-51. [DOI:10.1080/02701367.2003.10609063] [PMID]
- Cohen J. Statistical power analysis. Current Directions in Psychological Science. 1992; 1(3):98-101. [DOI:10.1111/1467-8721.ep10768783]
- Wist S, Clivaz J, Sattelmayer M. Muscle strengthening for hemiparesis after stroke: A meta-analysis. Annals of Physical and Rehabilitation Medicine. 2016; 59(2):114-24. [DOI:10.1016/j.rehab.2016.02.001] [PMID]
- Hafer-Macko CE, Ryan AS, Ivey FM, Macko RF. Skeletal muscle changes after hemiparetic stroke and potential beneficial effects of exercise intervention strategies. Journal of Rehabilitation Research and Development. 2008; 45(2):261-72. [DOI:10.1682/JRRD.2007.02.0040] [PMID]
- Lee MJ, Kilbreath SL, Singh MF, Zeman B, Davis GM. Effect of progressive resistance training on muscle performance after chronic stroke. Medicine and Science in Sports and Exercise. 2010; 42(1):23-34. [DOI:10.1249/MSS.0b013e3181b07a31] [PMID]
- Ouellette MM, LeBrasseur NK, Bean JF, Phillips E, Stein J, Frontera WR, et al. High-intensity resistance training improves muscle strength, self-reported function, and disability in long-term stroke survivors. Stroke. 2004; 35(6):1404-9. [DOI:10.1161/01.STR.0000127785.73065.34] [PMID]
- Janssen TW, Beltman JM, Elich P, Koppe PA, Konijnenbelt H, de Haan A, et al. Effects of electric stimulation− assisted cycling training in people with chronic stroke. Archives of Physical Medicine and Rehabilitation. 2008; 89(3):463-9. [DOI:10.1016/j.apmr.2007.09.028] [PMID]
- Tung FL, Yang YR, Lee CC, Wang RY. Balance outcomes after additional sit-to-stand training in subjects with stroke: A randomized controlled trial. Clinical Rehabilitation. 2010; 24(6):533-42. [DOI:10.1177/0269215509360751] [PMID]
- Lomaglio MJ, Eng JJ. Muscle strength and weight-bearing symmetry relate to sit-to-stand performance in individuals with stroke. Gait & Posture. 2005; 22(2):126-31. [DOI:10.1016/j.gaitpost.2004.08.002] [PMID]
- Nelson AG, Chambers RS, McGown CM, Penrose KW. Proprioceptive neuromuscular facilitation versus weight training for enhancement of muscular strength and athletic performance. Journal of Orthopaedic & Sports Physical Therapy. 1986; 7(5):250-3. [DOI:10.2519/jospt.1986.7.5.250] [PMID]
- Burke DG, Culligan CJ, Holt LE. The theoretical basis of proprioceptive neuromuscular facilitation. The Journal of Strength & Conditioning Research. 2000; 14(4):496-500. [Link]
- Bani-Ahmed A. The evidence for prolonged muscle stretching in ankle joint management in upper motor neuron lesions: Considerations for rehabilitation-a systematic review. Topics in Stroke Rehabilitation. 2019; 26(2):153-61. [DOI:10.1080/10749357.2018.1550958] [PMID]
- Le Sant G, Nordez A, Hug F, Andrade R, Lecharte T, McNair PJ, et al. Effects of stroke injury on the shear modulus of the lower leg muscle during passive dorsiflexion. Journal of Applied Physiology. 2019; 126(1):11-22. [DOI:10.1152/japplphysiol.00968.2017] [PMID]
- Jakubowski KL, Terman A, Santana RVC, Lee SSM. Passive material properties of stroke-impaired plantarflexor and dorsiflexor muscles. Clinical Biomechanics. 2017; 49:48-55. [DOI:10.1016/j.clinbiomech.2017.08.009] [PMID]
Type of Study: Research |
Subject:
Sport injury and corrective exercises
Received: 2023/11/20 | Accepted: 2024/07/20 | Published: 2024/10/1
Received: 2023/11/20 | Accepted: 2024/07/20 | Published: 2024/10/1
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |